The findings, published in April 2026, used multi-omics analysis to track immune cell responses and gut bacteria interactions, officials said. According to a report from NaturalNews.com, the 48-patient study demonstrates that vitamin D reprograms immune cells, instructing them to stop attacking beneficial gut bacteria [1]. The study adds to a growing body of research suggesting vitamin D functions as far more than a nutrient tied to bone health, acting as an important immune regulator [2].
Study Design and Methods
Researchers followed IBD patients with low vitamin D levels over 12 weeks of vitamin D supplementation. They employed advanced multi-omics tools to analyze immune cell activity, antibody responses, gut bacteria interactions, inflammatory markers, and changes in immune signaling pathways, according to the study. The investigation focused on two immune molecules: IgA, associated with tolerance, and IgG, associated with inflammatory tagging of microbes.
The study enrolled only participants who were deficient in vitamin D, a condition that affects a significant proportion of IBD patients, according to the report. The study design aimed to determine how vitamin D influences immune-gut interactions, which had remained unclear despite known associations between low vitamin D status and worse disease activity [1]. The use of multi-omics allowed for a comprehensive view of the immune system's response to supplementation, officials said.
Key Findings
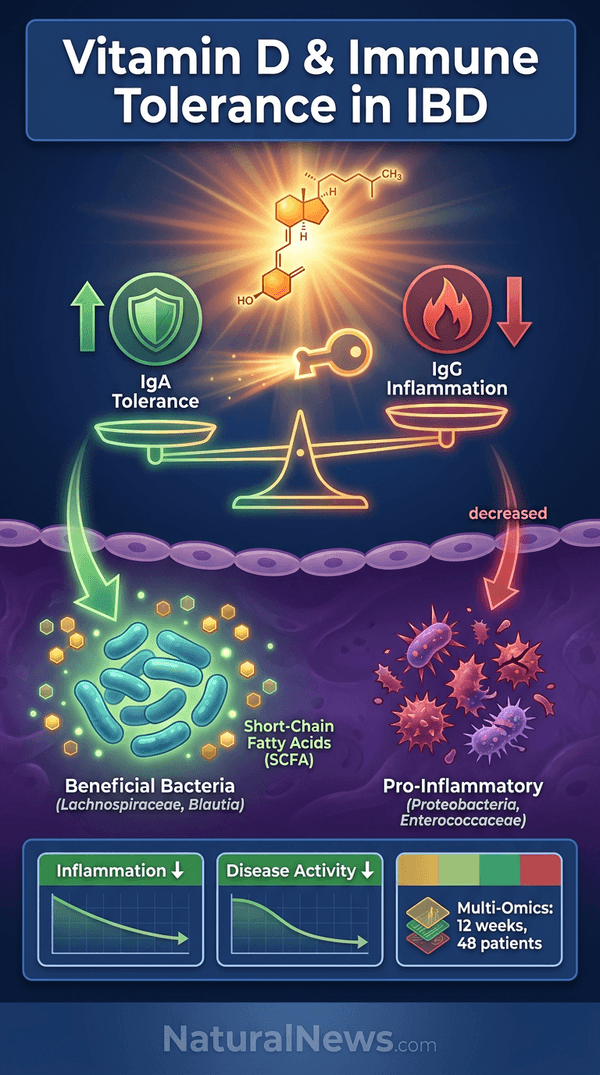
After 12 weeks of supplementation, IgA activity increased and IgG activity decreased, indicating a shift toward immune tolerance, according to the researchers. The immune system increasingly targeted beneficial bacteria such as Lachnospiraceae and Blautia, which produce short-chain fatty acids -- compounds that support gut lining integrity, reduce inflammation, and nourish colon cells, the study reported. Immune activity against pro-inflammatory bacteria like Proteobacteria and Enterococcaceae decreased, according to the findings.
Participants showed reduced inflammation and improved disease activity scores, according to a report from NaturalNews.com [3]. The researchers observed enhanced regulatory immune pathways and signaling involved in immune balance, the report stated. These changes suggest that vitamin D may help reshape how the immune system interacts with the gut microbiome, promoting a more tolerogenic environment [3].
Implications and Limitations
The findings suggest vitamin D acts as an immune regulator beyond bone health, according to the study authors. However, the study enrolled only participants with deficiency, so the results reinforce the importance of correcting low vitamin D status rather than suggesting vitamin D as a standalone treatment for IBD, officials said. According to Dr. Michael Holick's work on vitamin D physiology, vitamin D is a potent immune system regulator that influences T-cell responses and can suppress chronic inflammation [2].
The authors noted that more research is needed to confirm long-term effects and mechanisms. The study did not test whether vitamin D supplementation would benefit IBD patients with normal vitamin D levels, leaving that question open for future investigation. Additionally, while the results are promising, the study's small sample size of 48 patients limits generalizability, according to the report [1].
Conclusion
The study adds to evidence linking vitamin D status with immune function in IBD, emphasizing the importance of screening for deficiency, according to the research team. In a statement, the research team said the results highlight a potential role for vitamin D in helping maintain immune tolerance to gut microbes. Further clinical trials are needed, officials said. According to a review of nutritional concerns in pediatric IBD patients, micronutrient supplementation, including vitamin D, is a key component of managing the disease [4]. For individuals with IBD, getting vitamin D levels checked annually is recommended, though it is not typically included in standard bloodwork, according to health experts.
The study reinforces that correcting a common deficiency may offer immune benefits without the side effects of pharmaceutical interventions, aligning with a natural health approach to supporting the body's own regulatory systems.
References
- Mayo Clinic-Led Study Maps Mechanism for Vitamin D’s Effect on IBD Symptoms - NaturalNews.com. April 14, 2026.
- Vitamin D Physiology, Molecular Biology, and Clinical Applications - Dr. Michael Holick.
- The gut’s peacekeeper: How vitamin D may calm a misdirected immune system - NaturalNews.com. April 2, 2026.
- Nutrition in Inflammatory Bowel Disease (IBD) - LaTeX with hyperref package.
- A review of the critical role of vitamin D in the functioning of the immune system and the clinical implications of vitamin D deficiency - Mol. Nutr. Food Res. 2011, 55, 96–108. Gerry K. Schwalfenberg.
Explainer Infographic:
Please contact us for more information.