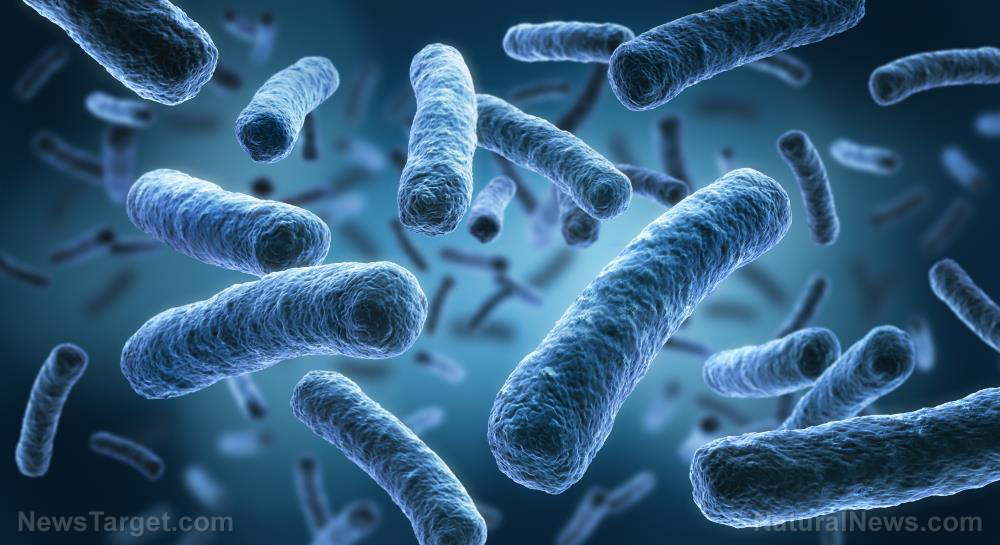
The gut contains trillions of microorganisms. Bacteria comprise most of the gut microbiota, but single-celled organisms and viruses are also present in considerable numbers.
Also called single-celled eukaryotes (SCE) and protozoans, single-celled organisms don't draw much attention from researchers. They're generally considered harmless.
However, a recent study by researchers from the National University of Singapore (NUS) showed that the protozoan Blastocystis might be harming good bacteria. By doing so, the eukaryote undermines gut health and health in general.
Blastocystis is a common protozoan and a parasite. It enters the human body either through the consumption of tainted food or water, or via physical handling of infected animals.
In the past, several experts hypothesized that Blastocystis can cause infections in the intestinal tract. However, some patients who have the parasitic protozoan still manage to remain healthy.
Hence, the NUS researchers focused on a local subtype of Blastocystis designated as ST7. Unlike its relatives, ST7 harms gut bacteria, including beneficial strains that contribute to good gut health. (Related: The “missing link” between gut health and undernutrition: Fermentable carbs and protein.)
A common protozoan harms good bacteria in the gut
For their experiment, the researchers took samples of Blastocystis ST7 from the stools of a patient with gastrointestinal issues. They kept two separate cultures of the protozoan: one with benign bacteria like Bifidobacterium longum and Lactobacillus brevis, and the other with bad bacteria like Escherichia coli.
The Bifidobacterium and Lactobacillus strains count as good bacteria. They help maintain the integrity of the intestinal lining.
Bifidobacterium helps break down dietary fiber and prevents infections. Meanwhile, Lactobacillus releases lactic acid that kills harmful bacteria in the intestine.
Both strains are popular choices for probiotic supplements. People often take them to improve their gut health.
Published in the scientific journal Microbiome, the NUS study reported that the presence of Blastocystis ST7 affects the balance of gut microbiota. The protozoan encourages the growth of some bacteria and kills off beneficial strains.
Mixing good gut bacteria with Blastocystis ST7 led to the death of both Bifidobacterium and Lactobacillus. This took place in both cell cultures and in animals.
Blastocystis ST7 helps bad bacteria and causes inflammation in the gut
The NUS researchers attributed the demise of the good bacteria to the production of reactive oxygen species. These harmful molecules are toxic to cells and bacteria.
The body releases reactive oxygen species when it experiences oxidative stress. This kind of stress occurs when free radicals outnumber the natural antioxidants that usually scavenge them.
The researchers also reported that Blastocystis ST7 supports the growth of E. coli, a strain of harmful bacteria that can cause deadly infections.
In addition, the protozoan damages the intestinal lining. Besides killing off good bacteria that protect this lining, ST7 triggers inflammatory responses in the gut. This leads to ulcers and further weakens the gut lining.
“This is the first detailed study to show a causal link between Blastocystis, a common [SCE] of the human gut, and the host microbiota,” stated NUS researcher Kevin Tan. “We reveal how it reduces the numbers of beneficial bacteria, which may, in turn, lead to an unbalanced gut microbiome and poorer gut health."
Blastocystis ST7 infections mostly occur in Singapore, but some cases have also been reported in Denmark and Japan. The NUS researchers recommend more studies to figure out if this harmful protozoan subtype exists in other areas.
Conventional treatment involves taking the pharmaceutical drug metronidazole. However, the ST7 subtype resists the effects of the antibiotic. Researchers are now looking for alternative treatments.
Sources include:
Please contact us for more information.




















