In their paper, the researchers looked at the enzyme diacylglycerol acyltransferase 1 (DGAT1) and how inhibiting its production affects the body. DGAT1 is a fat-synthesizing enzyme that is present in the liver and is associated with the production of very low-density lipoprotein (VLDL). DGAT1 protects cells from damage caused by lipotoxic stress during adipocyte lipolysis. By mediating fatty-acid re-esterification, DGAT1 averts ER stress and lipotoxicity.
DGAT1 is not only linked to synthesizing fat: A study published in The Journal of Biological Chemistry concluded that the enzyme also plays a role in maintaining healthy skin and hair. In their study, researchers from the Gladstone Institutes of Cardiovascular Disease found that removing DGAT1 in mice causes an increase in retinoic acid levels in the skin, which leads to hair loss. In itself, retinoic acid is beneficial – it's been known to reduce fine lines and wrinkles – but without DGAT1, it becomes unregulated. Retinol is toxic if it is not controlled, and without DGAT1, it can cause increased sensitivity to the skin and even alopecia.
The current study, led by Victor Zammit from Warwick Medical School, established how inhibiting DGAT1 in the liver can reduce the size of VLDL particles – including their triglyceride content – by nearly half, demonstrating the role that it plays in "loading up" VLDL with fat. While VLDL carries triglycerides to the tissues for storage, having elevated levels of it in the body can increase the risk of coronary artery disease. The amount of fat that VLDL particles carry determines their size: The larger they are, the more "bad" the cholesterol in them becomes.
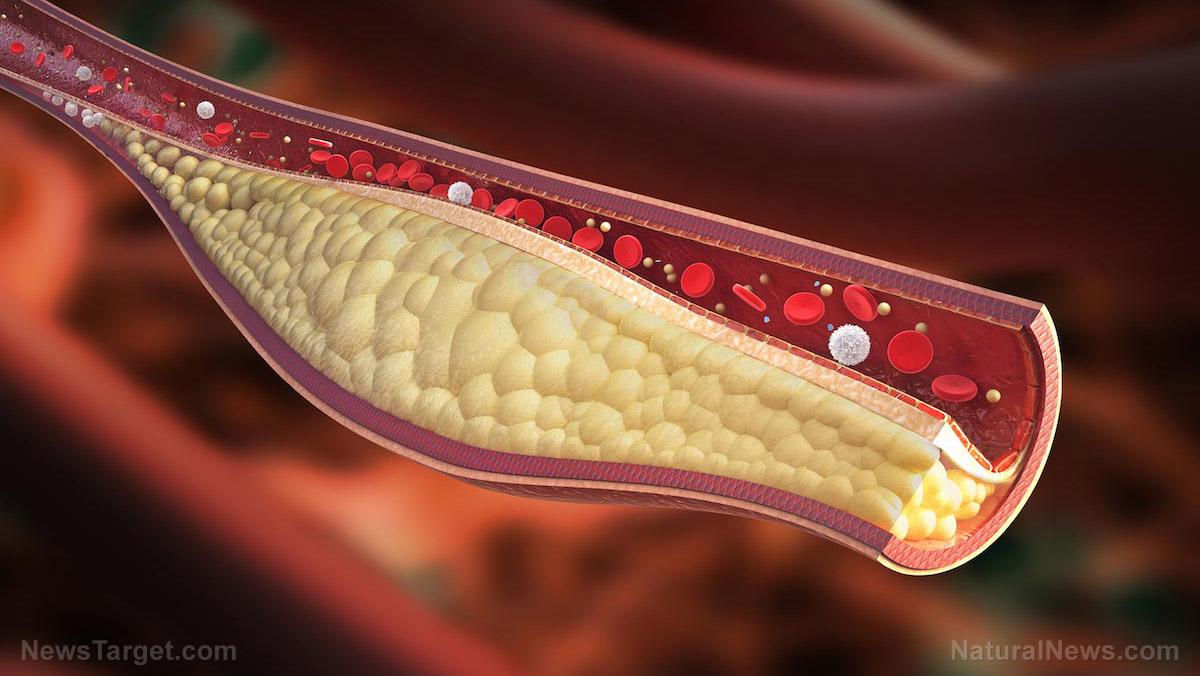
"VLDL particles themselves are not harmful but when they are depleted of triglyceride after they offload it to other tissues, they become Low-Density Lipoprotein which are the carriers of 'bad' cholesterol," Zammit explained. "This is the cholesterol that is associated with heart disease as the LDL deposit it within the walls of arteries, resulting in arteriosclerosis which can result in blockage of the coronary arteries with an associated increased risk of heart attacks and strokes."
The researchers also noted that while inhibiting DGAT1 levels in the liver did not cause significant changes in the number of particles, it did cut triglyceride content by half. Having high levels of triglycerides in the body – 200 milligrams per deciliter or above – is a risk factor for chronic diseases like heart disease and metabolic syndrome. It also causes VLDLs to increase in size, which makes them become more "sticky" and more likely to build up in the vascular lining, resulting in atherosclerosis.
"Our findings identify the enzyme (DGAT1) as the key determinant of the content of triglycerides, and therefore the size, of VLDL particles," Zammit noted. (Related: New research shows blueberries lower LDL cholesterol better than statin drugs.)
"Bad" cholesterol can even cause dangerous blood clots
Aside from being a risk factor for chronic illnesses like cardiovascular disease, "bad" cholesterol can also increase a person's risk of getting a potentially dangerous blood clot known as venous thromboembolism (VTE). In a study presented in the American Health Association's Vascular Discovery Scientific Session, researchers obtained data from the Department of Veteran's Affairs' Million Veteran Program and the U.K. Biobank. They tested for 13 million genetic variants and found new factors that contribute to VTE, including a protein called plasminogen activator inhibitor 1 and low-density lipoprotein (LDL) cholesterol.
For Dr. Scott Damrauer, a researcher from the University of Pennsylvania, this finding highlights the role of cholesterol in venous disease. The condition is considered an important cause of cardiovascular death and disability worldwide, with over a million people in the U.S. suffering from the condition. According to the Centers for Disease Control and Prevention, VTE is also the leading cause of preventable death among hospital patients in the country. Read on to learn why you should never take statin drugs to reduce cholesterol levels.
Sources include:
Please contact us for more information.