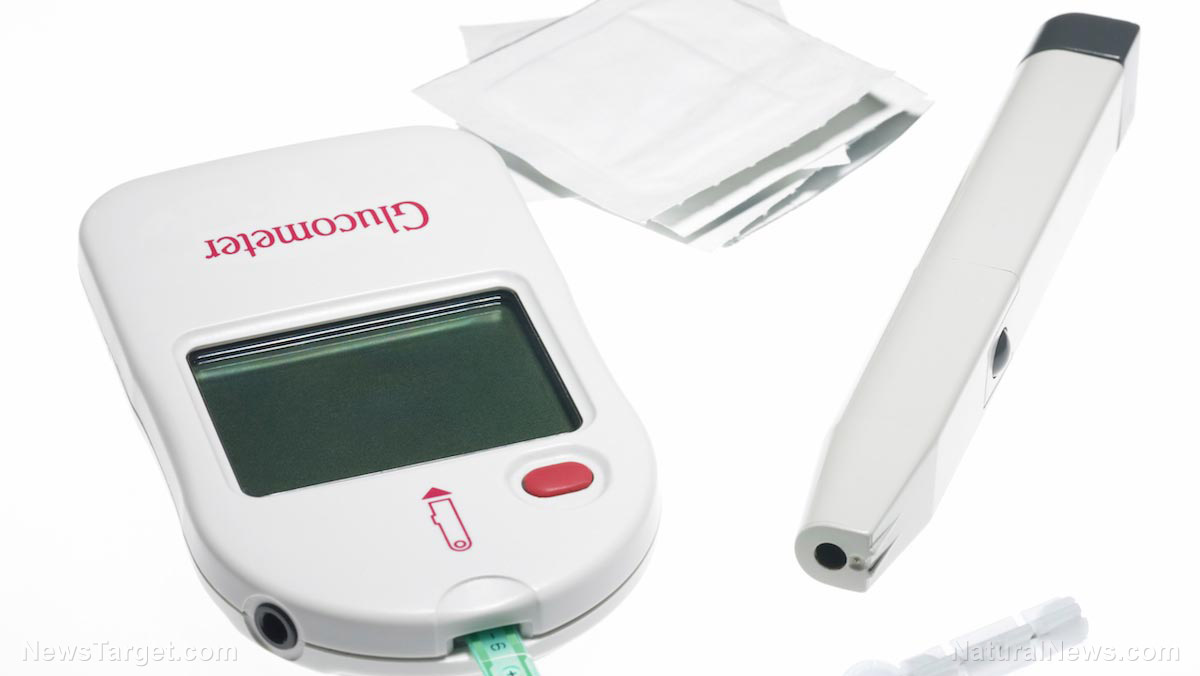
The new device was designed by researchers at the Oregon State University for those who suffer from Type 1 diabetes, a condition that 1.25 million Americans have. These people must monitor their glucose levels and are often forced to take hormone therapy when they least expect it.
In Type 1 diabetes, the pancreas is mistaken for a pathogen by the immune system. The important organ gets besieged by antibodies and becomes unable to send out hormones that regulate glucose levels in the blood.
One out of every 20 diabetics suffers from this type of diabetes. Many of these cases are diagnosed during youth, which leads to the disease being called "juvenile diabetes." (Related: Whole grains offer an easy way to prevent Type 2 diabetes.)
"Artificial pancreas" tracks glucose levels and pumps insulin as needed
The researchers used a 3D printer to place glucose sensors onto a catheter that is then connected to a wearable pump. The transistors and biosensors are transparent electronic systems that do not disturb the smooth curves of the glass tube.
When the sensors detect a spike in blood glucose, the pump will send insulin and glucagon into the bloodstream of the user. The hormones will reduce the sugar to the normal concentration.
Many Type 1 diabetes patients are wearing pumps like this. The addition of glucose sensors to the catheters automates the chore and takes that load off the user's mind.
The upgraded wearable device will serve as an artificial pancreas that doesn't have to be installed or transplanted inside the body of the patient. It will perform the disabled organ's duties of managing the amount of sugar in the blood and getting usable energy from food.
The glucose sensors in the catheter will perform two roles. In addition to keeping track of the diabetic's blood sugar level, it will also keep the programmable pump informed as to when it should release insulin and glucagon into the bloodstream.
Microcontact printing puts tiny sensors on the thin catheter of the insulin pump
The study builds off an earlier attempt by the same Oregon State researchers to add sensors to a catheter tube. In that prototype, they put the glucose sensors on a polymer film. Then they wrapped the film around the catheter.
During animal testing, the arrangement proved to be fragile. Either the sensors ended up separating from the film, or the latter peeled off the catheter. Both outcomes were dangerous for the animal wearing the catheter.
While their collaborators chose to make the glucose sensors stronger in their own pursuit of the matter, the researchers implemented a different solution. They put an amorphous indium gallium zinc oxide, field-effect transistor (a-IGZO-FET) onto a glass tube that measures one millimeter across.
Furthermore, they used microcontact printing to put the sensor on the catheter. This new printing technique had no problem putting the pattern on the highly curved surface of the tube.
"The process takes advantage of an elastomeric stamp’s ability to conform to curved substrates with minimal distortion of the printed pattern," the researchers reported in their study. "The adhesion of the deposited films to the glass tube is very good."
Their next plan is to fabricate a-IGZO-FET sensors on an optical fiber. If successful, they could enhance the sensitivity of endoscopes and other optical sensing systems that also need to be flexible.
Sources include:
Please contact us for more information.


















