"Patients with NAFLD and NASH have had limited treatment options for years. What the results of our phase II study show is a promising future where NGM282 may be able to provide relief to these patients," explained Dr. Rohit Loomba, the study's senior author and a director of hepatology at the University of California, San Diego School of Medicine.
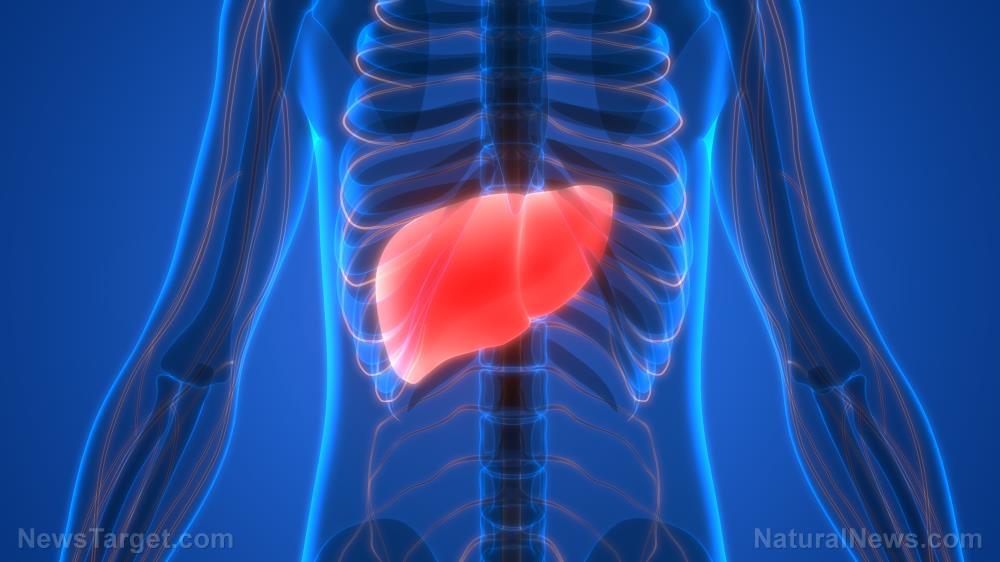
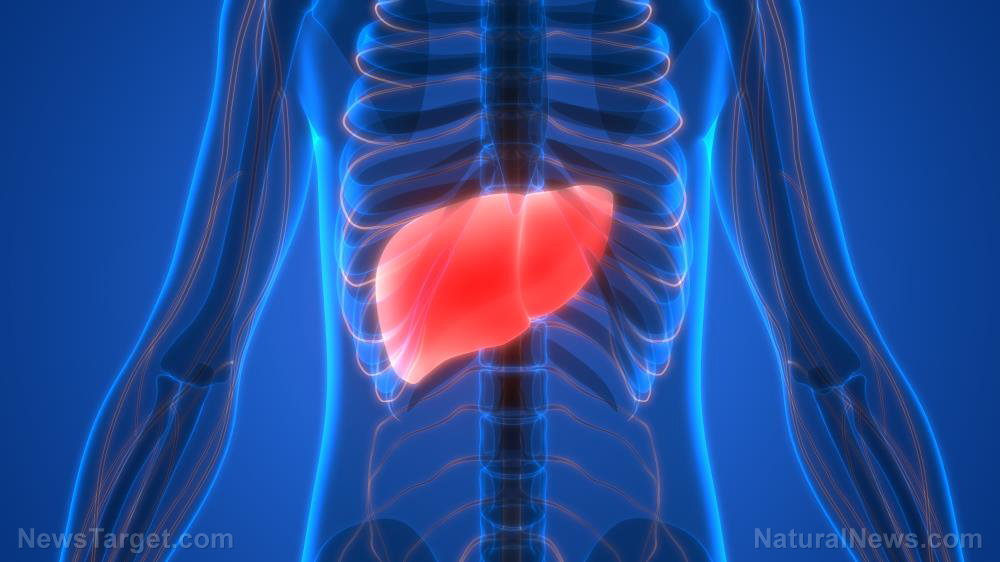
NALFD is a common cause of liver disease in the U.S., with up to 40 percent of adults having the condition. According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), the term NAFLD refers to a condition marked by excess fat droplets in the liver that's not caused by heavy alcohol use.
There are two main types of NAFLD: simple fatty liver and NASH. In simple fatty liver, also called non-alcoholic fatty liver (NAFL), the liver already contains excess fat; however, there is little to no inflammation in the liver. NASH is a different story altogether: Aside from the fat buildup, the liver also suffers from noticeable inflammation and fibrosis (scarring). (Related: Treat non-alcoholic fatty liver disease naturally.)
According to the researchers, NAFLD could mean any number of chronic liver disease, with NASH being its most aggressive type. The causes of both NAFLD and NASH are not completely understood, but certain risk factors like obesity and Type 2 diabetes increase the likelihood of getting the disease.
For the study, the team employed a randomized, double-blind, placebo-controlled phase II clinical trial. Over 160 individuals were recruited for the study from 18 hospitals, gastroenterology, or liver clinics in the U.S. and Australia. Everyone who took part in the trail either had been diagnosed with either NAFLD or NASH and have a liver fat content of at least eight percent. They also had a score of four or higher in the non-alcoholic fatty liver score, and have also exhibited either stage 1 to 3 fibrosis.
Patients were then randomly assigned using a web-based computer system. Based on the status of their diabetes, they either received a 3 mg or 6 mg injection of NGM282 or a placebo once a day. Researchers checked in with participants twice a week over a three-month period. They measured reductions in liver fat through hepatic MRIs with proton density fat friction – an imaging type that can better pick up changes in liver composition than traditional methods of tissue sample analysis.
Researchers then looked at data from before the treatment (considered the baseline) to measurements by the end of week 12. For a procedure to be considered effective in a patient, his overall liver fat content must drop by five percent or higher. Based on the results of the study, at least 70 percent of participants who took NGM282 had a five percent drop in their liver fat content from baseline after the treatment. This was true for both 3 mg and 6 mg doses.
After looking at the results of the trial, researchers concluded that NGM282 quickly and significantly reduced the liver fat content in patients with non-alcoholic steatohepatitis.
"Moving forward, we are continuing the development of this compound for the treatment of NASH-related fibrosis," added Loomba. "In this, we hope to further examine the efficacy of this hormone in improving liver histology based end-points in patients with biopsy-proven NASH with fibrosis."
NGM282 is the lead product of NGM Biopharmaceuticals, which funded the study. In their website, they explained NGM282 as "a first-in-class, non-tumorigenic, engineered variant of the human hormone FGF19 that dramatically reduces liver fat content and improves liver function by targeting multiple pathogenic pathways of nonalcoholic steatohepatitis (NASH)."
Sources include:
Please contact us for more information.