The diseases have different origins. Lyme disease is a bacterial disease caused by the bacteria Borrelia burgdorferi, which infect humans via tick bites. Meanwhile, rheumatoid arthritis stems from a mixture of environmental factors, genetics, and earlier infections.
Both diseases cause headaches, fatigue, and pain and swelling in the joints. The symptoms appear early in Lyme patients and may come with a rash. They may also vanish for a while before returning much later as the bacterial infection enters its later stages.
The later stages of Lyme disease may involve the joints. The resulting "Lyme arthritis" shows symptoms similar to rheumatoid arthritis, making it possible for people to mistake one for the other.
Since Lyme disease is a bacterial infection, it is curable with a treatment period that ranges from months to years. In contrast, rheumatoid arthritis is a chronic condition. (Related: Ozone therapy is an ideal alternative to treating Lyme disease.)
Telling Lyme disease apart from rheumatoid arthritis
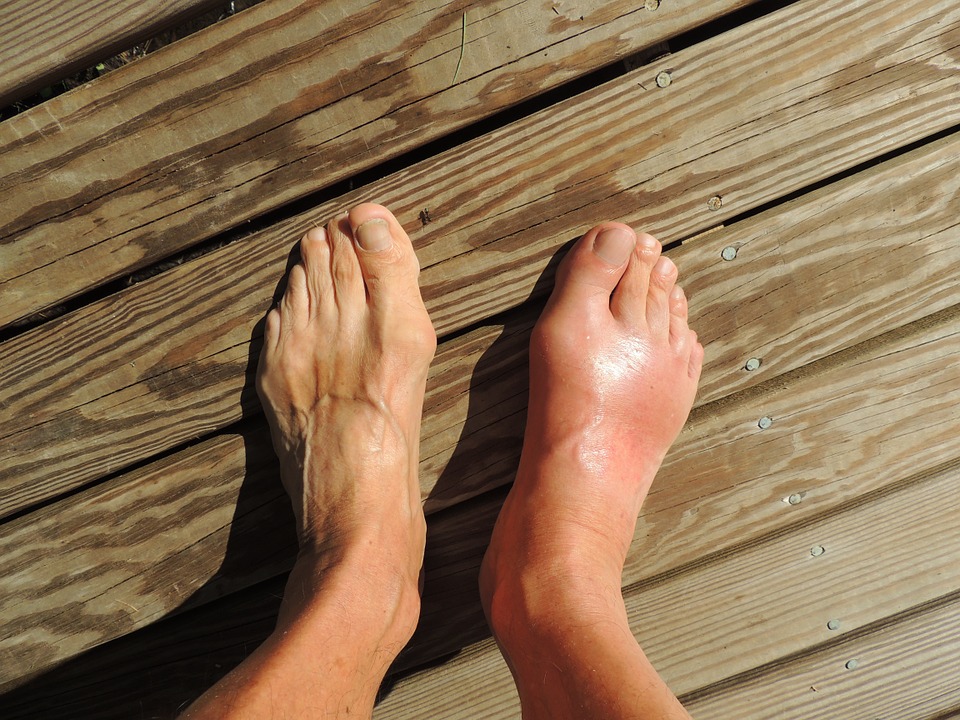
One easy way to tell them apart is that Lyme arthritis usually targets the knees. In comparison, rheumatoid arthritis often affects the hands and feet – the discomfort and pain start at the joints of the fingers and toes before spreading out.
On occasion, rheumatoid arthritis also strikes the knees. When that happens, it becomes likely to get mistaken for Lyme arthritis.
Thankfully, it is easy to distinguish between rheumatoid arthritis of the knees and Lyme arthritis.
In 2015, Harvard Medical School researchers reported that Lyme disease rarely causes symmetrical arthritis. That means Lyme arthritis usually restricts itself to one joint on one side of the body.
The restriction to one side differentiates late-stage Lyme disease from rheumatoid arthritis. The chronic condition usually affects the joints equally on both sides of the patient's body.
Further, while Lyme arthritis causes discomfort, it rarely causes severe pain when the patient moves his joints. It is less painful and immobilizing than rheumatoid arthritis.
Possible treatments for Lyme disease
The timing when the patient gets diagnosed with Lyme disease will determine the treatment he receives. If healthcare providers diagnose the disease during its earlier stages, they will recommend antibiotic treatment for the bacterial infection.
Early treatment of Lyme disease will usually prevent late-stage Lyme arthritis from bothering the patient later on. Antibiotic therapy will help the immune system expel the B. burgdorferi bacteria from the body.
If a patient receives a late diagnosis and develops Lyme arthritis, the healthcare provider may recommend an extended course of antibiotic therapy. However, the prolonged use of antibacterial pharmaceutical drugs may lead to adverse effects.
Natural alternatives include eating mushrooms and garlic. Patients may also take herbal remedies made from valerian root, passionflower, or Echinacea.
Treatments and remedies for rheumatoid arthritis
As for rheumatoid arthritis, the appropriate treatment depends on the severity of its symptoms. Physicians may prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) for the early stages of the condition. For severe cases, they may recommend disease-modifying anti-rheumatic drugs (DMARDs) and biologics. However, all these pharmaceutical drugs cause many side effects – taking large amounts for long periods will lead to more health problems.
Home remedies for rheumatoid arthritis include plenty of rest, meditation, yoga, physical exercise, a gluten-free diet with fresh and natural foods, essential oils, herbal remedies and teas, hot baths, hot and cold packs, massage, and fish oil supplements.
Rheumatoid arthritis doesn't have a cure yet. However, patients may stop the condition from growing worse, thereby reducing the harm done to their health.
Sources include:
Please contact us for more information.