Unsurprisingly, arthritis sub-types comprise half of the 12 likeliest suspects for misdiagnosis of rheumatoid arthritis. Rheumatoid arthritis belongs to the autoimmune or inflammatory sub-type. There are also degenerative, infectious, and metabolic sub-types of arthritis.
Rheumatoid arthritis may be mistaken for other sub-types of arthritis
Lupus became famous after its regular mention on the show "House." This autoimmune disease targets many parts of the body that are also affected by rheumatoid arthritis. The best way to differentiate them is to gauge the intensity of their symptoms. Rheumatoid arthritis is more intense than lupus.
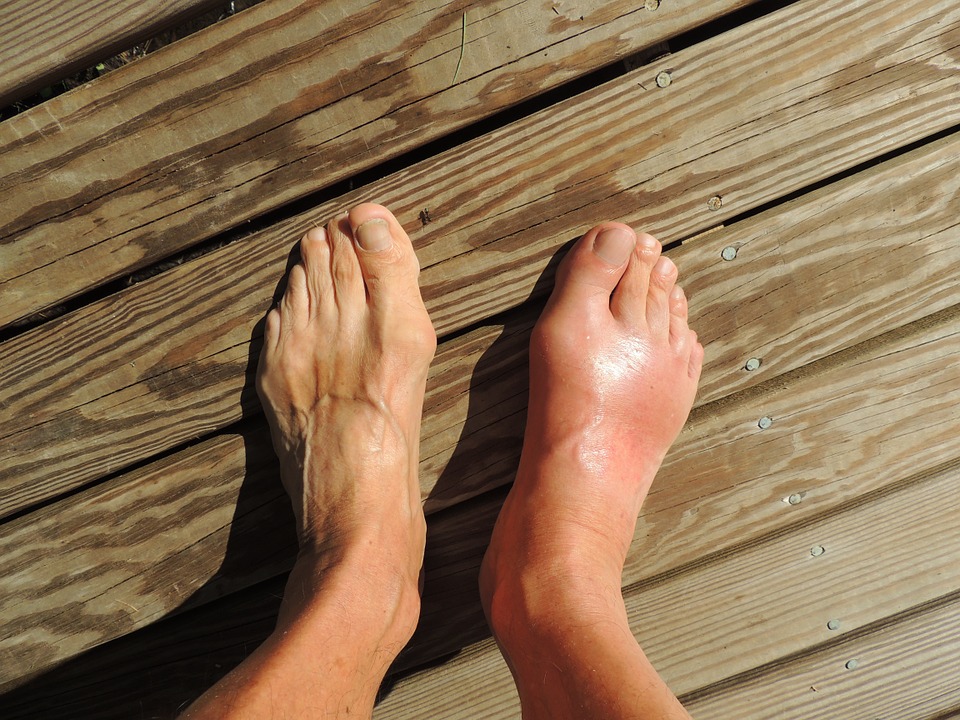
Gout is more difficult to distinguish from rheumatoid arthritis. Like the latter, it also causes erosive and deforming arthritis. Further, patients with gout develop trophi – deposits of tissue around the joints that resemble rheumatoid nodules. But while rheumatoid arthritis is an autoimmune disorder, gout comes from unhealthy levels of uric acid in the blood.
As its name implies, pseudogout resembles gout. Patients undergo severe episodes of inflammation in the synovial membrane that borders joints. Some of the clinical manifestations of this synovitis resemble the symptoms of rheumatoid arthritis.
Ankylosing spondylitis takes place within the connections of the spinal column. It causes inflammation that leads to severe back pain when the patient wakes up, although the pain tapers off as the day progresses.
Also known as reactive arthritis, Reiter's syndrome belongs to the infectious sub-type of arthritis. It arises from exposure to disease-causing bacteria, although it may take a while before its symptoms start appearing. Patients with Reiter's will experience inflammation and swelling in several joints. Usually, the affected joints are limited to one side of the body.
Thankfully, Reiter's syndrome only lasts for a few months. On the other hand, rheumatoid arthritis will never go away and requires management.
Osteoarthritis is the final arthritis sub-type that may get mistaken for rheumatoid arthritis. Unlike the previous examples, it doesn't share the same signs and symptoms, affects different joints, and mainly affects older people (who can keep it away by walking 10 minutes a day).
The exemption is erosive osteoarthritis. It may appear inflammatory to the eyes of a healthcare professional, which may lead to a misdiagnosis of rheumatoid arthritis. (Related: Natural treatment for rheumatoid arthritis: Research shows yoga can relieve physical and psychological symptoms.)
Non-arthritis diseases that may get misdiagnosed as rheumatoid arthritis and vice versa
Some non-arthritic diseases may feature symptoms that resemble those of rheumatoid arthritis. For example, the early stages of Lyme disease cause inflammation and pain in the joints and muscles of patients. However, as the tick-borne disease progresses, it causes inflammatory arthritis in the joint of one of the lower limbs. Rheumatoid arthritis, in comparison, affects the same joint on both extremities.
Scleroderma and rheumatoid arthritis both test positive on lab tests for creatine kinase measurements, erythrocyte sedimentation rate, and C-reactive protein – the comparable results stem from their shared nature as autoimmune diseases.
Inflamed blood vessels characterize the disease called vasculitis. The systemic type may lead to polyarthritis. Other subtypes may test positive for the rheumatoid factor that indicates rheumatoid arthritis.
Sjogren's syndrome is another autoimmune disease with similar clinical symptoms and test results to rheumatoid arthritis. Many patients may show positive results for the rheumatoid factor.
Patients with sarcoidosis develop the same synovitis as pseudogout, which may get mistaken for rheumatoid arthritis. The disease does possess unique characteristics that make it easier to detect.
Finally, fibromyalgia mimics the discomfort and stiffness in the joints that describe rheumatoid arthritis. But it doesn't inflame the blood vessels and causes no pain during movement.
Learn more about rheumatoid arthritis and other inflammatory diseases at Health.news.
Sources include:
Please contact us for more information.