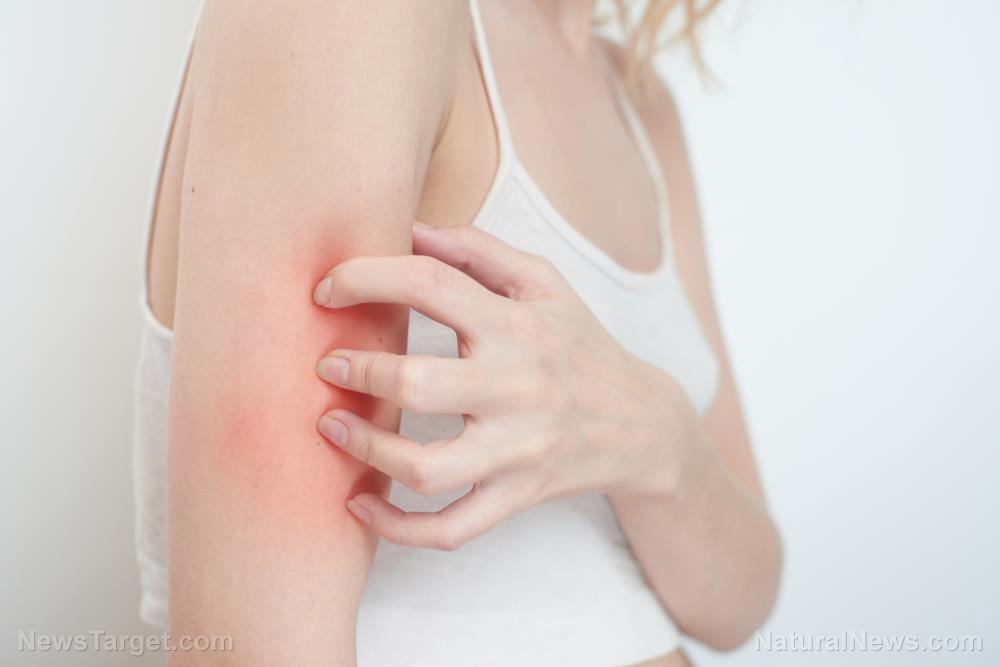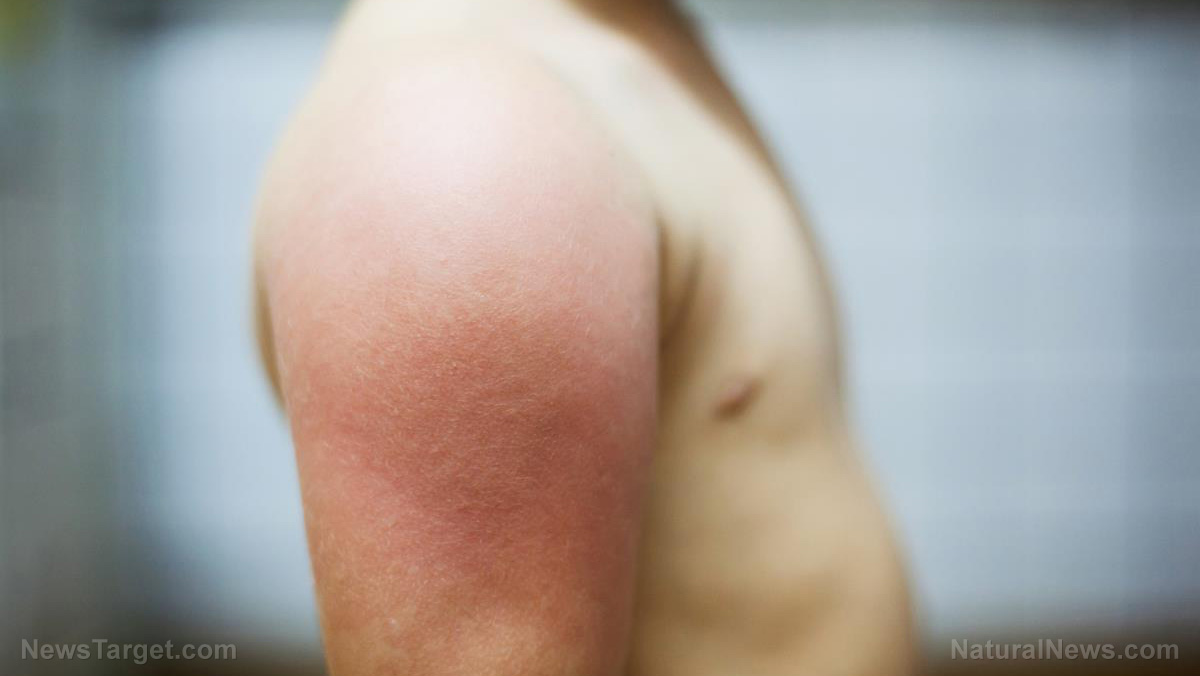
An ongoing clinical trial led by researchers from the NIH's National Institute of Allergy and Infectious Diseases (NIAID) has potentially good news for all those who suffer from the disease. It appears that the solution lies in the application of live bacteria to the skin. According to the study, positive strains of a bacterium called Roseomonas mucosa or R. mucosa, which naturally lives in the skin, brings relief to eczema's symptoms.
Although the main cause of eczema has not been determined yet, doctors believe that the disease has something to do with a person's skin microbiome -- a community of bacteria and microbes. Furthermore, after comparing recent and previous studies, the researchers saw a pattern in the skin that shows gram-negative bacteria like to grow in areas where eczema usually thrives -- such as the elbow folds and the back of the knees. They suspected that the "wrong" kind of bacteria may be causing eczema.
To test their theories, the study's authors took strains of R. mucosa from people who have healthy skin and injected it into a mouse subject. Results showed that the good bacteria improved the barrier function of the mouse's skin. The skin had better abilities in sealing moisture, keeping allergens from entering the body. R. mucosa was also found to be effective in killing a bad bacterium called Staphylococcus aureus, which causes skin infection, increases inflammation, and worsen symptoms. (Related: Compounds in marijuana may be helpful in alleviating symptoms of eczema and psoriasis.)
In order to solidify their findings, researchers initiated an early stage clinical trial involving 10 adult volunteers. The participants were sprayed with a solution of sugar water with increasing doses of live R. mucosa on their elbow folds and another skin area of their choice. This was done two times a week for one and a half months. The strains of R. mucosa came from the skin of healthy individuals and grown under controlled laboratory conditions.
All volunteers continued to use their regular eczema medications during the experiment. Although not all participants experienced positive effects, no one displayed any negative side effects. Moreover, four weeks after receiving sprays of live bacteria, some reported needing less topical steroids.
Researchers then did the experiment on five kids, aged between nine and 14. The solution was applied twice a week for three months and every other day for another four weeks. Similar to the adult group, there were no complications and most of the kids' conditions improved.
"By applying bacteria from a healthy source to the skin of people with atopic dermatitis (eczema), we aim to alter the skin microbiome in a way that will relieve symptoms and free people from the burden of constant treatment," NIAID’s Ian Myles, M.D., lead trial investigator, said. "If future clinical studies demonstrate that this strategy is effective, we hope our work will lead to the development of new, low-cost atopic dermatitis therapies that do not require daily application."
During the study, researchers also found that some skin products and topical creams contain parabens that block the growth of R. mucosa. This finding hints that some products used on the skin may worsen eczema and/or affect the effectiveness of microbiome-based therapies.
The researchers are planning on conducting a larger study on the matter, possibly involving hundreds more of volunteers, to see if there's a possibility of releasing the treatment to the public.
Find more medical breakthroughs by visiting Research.news today.
Sources include:
Please contact us for more information.