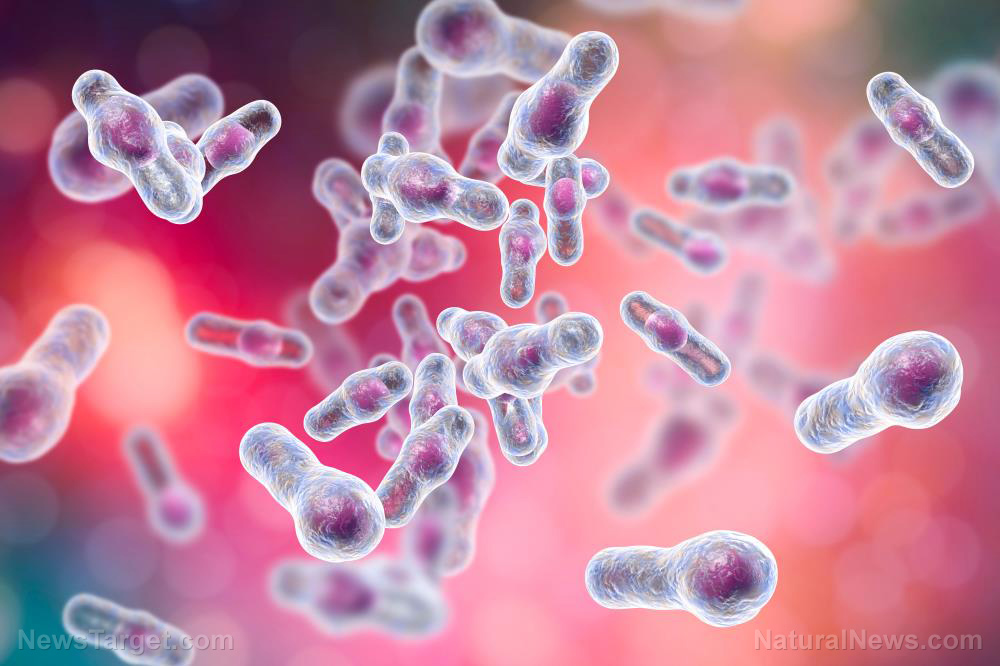
The two individuals were exposed to contaminated water spray and while this might seem shocking, experts say that these incidences aren't that rare.
Dr. Tom Makin, a microbiologist from the United Kingdom, explains that car washes can produce the right-sized aerosols that can be inhaled into the lungs where the Legionella bacteria can cause an infection like pneumonia.
Dr. Makin adds that while this is no cause for panic, especially for a Legionnaires' threat at car washes, proprietors can be more aware of the situation if possible risk situations are flagged immediately. Management and employees, who are regularly exposed to water aerosols as an occupational hazard, and the general public who frequent these businesses, will also benefit from warnings about these risk situations.
To prepare the public against potential Legionnaire's disease outbreaks, the focus must be on education instead of scaremongering. Even though it's mostly true that water sources which produce aerosols/sprays are possible transmitters of the bacterium, such as car washes, regular maintenance, and risk management can help curb the spread of any disease. (Related: Legionella bacteria in municipal water systems has killed or sickened thousands – is anything being done to address the problem?)
The disease can also spread via shower heads, spas, swimming pools, or other systems that disperse water via a building’s ventilation system. A water storage facility that might house stagnant or temperature-fluctuating water can also act as a breeding ground for Legionella bacteria. Take note that any equipment which creates microscopic water droplets, which can be inhaled, is a danger to public health.
How can car wash proprietors prevent the spread of Legionnaires’ disease?
There are several ways to minimize the risk of Legionnaires' disease, such as:
- Systematically checking and disinfecting filtration equipment, interceptor tanks, and water collection while also establishing the regular rule over the current treatment system.
- Organizing a biocide (poisonous substance, e.g. pesticide) program to educate those who are responsible for risk control in the workplace about the importance of monitoring established systems, along with the possible switch to environments controlled in the same way like cooling towers are.
- The regular cleaning and disinfection of systems and proper emptying of sludge tanks.
- Legionella samples must be taken quarterly to gauge the effectiveness of risk management, or "as agreed/indicated by dedicated risk assessment practices in situ".
What is Legionnaires’ disease?
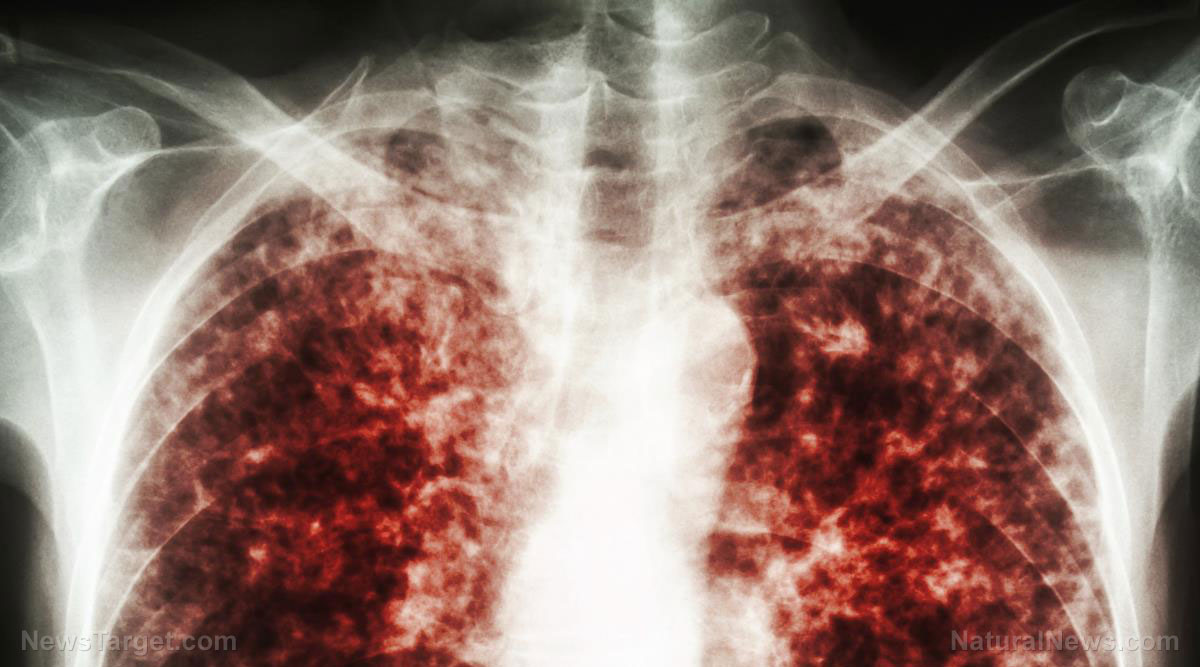
Legionnaires' disease is a severe form of pneumonia that causes lung inflammation. The disease is caused by a bacterium called Legionella. At least 500 people in the U.K. and 6,100 in the United States are infected by the bacteria yearly.
The disease can often lead to fatal complications such as kidney or respiratory failure and septic shock, which occurs when blood flow to the vital organs is blocked. Most patients develop Legionnaire's disease once they inhale tiny water droplets from infected sources like shower heads or ventilation systems in buildings.
While anyone can get infected, those at risk include the elderly, smokers, and those with suppressed immune systems (e.g. chemotherapy patients).
The symptoms of Legionnaires' disease often develop at least two to 10 days following exposure to the bacteria. Early symptoms include:
- Fever and chills
- Headache
- Muscle pain
After the symptoms mentioned above, patients may experience:
- Breathlessness
- Chest pain
- Confusion
- Coughing or hemoptysis (coughing up blood)
- Nausea, diarrhea, or vomiting
The disease is treated with antibiotics, which are often administered in the hospital.
The spread of Legionnaires' disease can be prevented with the thorough cleaning and disinfection of water systems. Individuals can also reduce their risk by not smoking, which damages the lungs and makes one more susceptible to infection.
You can read more articles about water safety and how to avoid harmful water pollutants at Cleanwater.news.
Sources include:
Please contact us for more information.