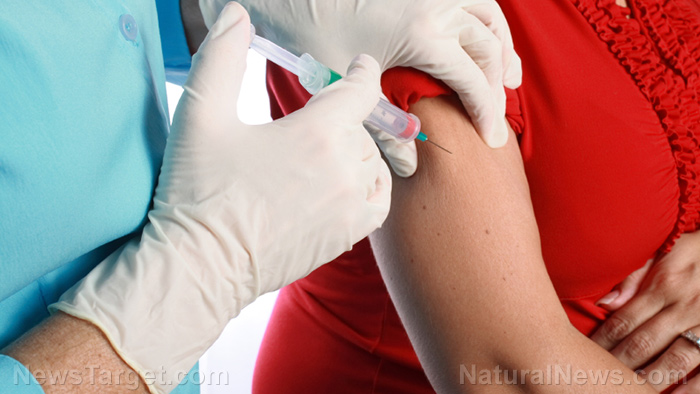
The following is a rebuttal to an article on Natural News entitled UV light treatments found to slash hospital superbug infections by 30%, which touted the benefits of a UV treatment technology to eliminate superbugs in hospitals. A competing manufacturer of UV treatment devices says the press release upon which that story was based is misleading, so we gave them an opportunity to tell their side of the story. What follows is their perspective on this issue.
Healthcare associated infections (HAI) have become one of the leading causes of death in the United States, killing as many people each year as AIDS, breast cancer and automobile accidents combined. Current CDC statistics show that in the U.S., one in every 25 patients will contract an HAI and of those, one in nine will die.
Devastating microbes like methicillin-resistant staphylococcus aureus (MRSA), Clostridium difficile (c. diff) and Acinetobacter baumannii often kill patients -- turning routine and potentially positive outcomes into debilitating and costly healthcare nightmares costing the industry close to $30 billion annually.
The rush to find a solution to this infection epidemic has led some companies to release misleading information about the efficacy of their products. For example, a CDC-funded study published earlier this year in the Lancet1 evaluated the effect of a mercury ultraviolet (Mercury UV) device on room disinfection, and specifically its impact on C. diff., MRSA, Acinetobacter and VRE infection rates. According to the Lancet study, there was no decrease in C. diff infections when the mercury UV device was used and no statistically significant decrease in MRSA infections2. There was a 30 percent decrease in VRE infections (when the device was used with bleach) and no changes in Acinetobacter infections yet Tru-D, the maker of the mercury UV device, issued a press release claiming, “The study proves that Tru-D can cut transmission of four major superbugs among patients admitted to the same room by a cumulative 30 percent.”3

C. diff and MRSA infections are two of the most common and deadly hospital acquired infections, and most hospitals that purchase UV disinfection technology do so to combat C. diff. and MRSA. Tru-D’s statement is clearly misleading, as it implies that the study proved effectiveness against the four superbugs, when in fact the study showed no impact on three of the four pathogens. The company’s brazen attempt to mislead hospital executives about product efficacy that can be a matter of life and death for patients is shocking.
In October, the Environmental Protection Agency (EPA), a regulatory agency for the room disinfection industry, sent a cease and desist letter to the same mercury UV vendor, Tru-D, telling the company to immediately:
-
Stop using the EPA logo
-
End its practice of claiming that “the EPA endorsed Tru-D Lamps”
-
End its practice of claiming that “Tru-D Bulbs are manufactured by Phillips Healthcare, which is endorsed by EPA and DOE.”
-
Cease its use of the EPA mark, including the removal of the EPA mark from its website, brochures and other print media, and to cease disseminating print media that contains the EPA mark.
Many UV disinfection manufacturers, including Tru-D, use mercury bulbs in their devices. Some of them do not disclose that their bulbs contain toxic mercury, and many of them do not provide safety precautions that should be followed when using mercury bulb devices. It is well documented that the chemical element mercury is toxic to the central and peripheral nervous systems. Special handling is required if mercury bulbs break and special disposal requirements may apply depending upon the amount of mercury present in the bulb and the state where the bulb is disposed. A study by the Maine Department of Environmental Protection tested the levels of mercury vapor that persist after a single compact fluorescent lamp breaks and found that mercury concentration in the room could exceed 300 times the state limits, especially at lower heights where children could inhale the mercury vapor.
There are other risks for hospital workers as well. Mercury UV devices contain 4-27 mercury bulbs, depending on the device design. Some mercury UV disinfection equipment requires warm-up and cool down times, as the bulbs may reach 220 degrees and should not be moved until the bulbs cool to a safe temperature.
Shortly after its warning from the EPA for its untruthful statements, Tru-D was notified by the Department of Veteran Affairs (VA) to cease making false statements regarding a VA employee, Dr. Chetan Jinadatha. Dr. Jinadatha is a highly respected researcher employed by the VA who has reported favorably on a non-mercury UV competitor of Tru-D. Tru-D’s mercury bulbs produce continuous, single spectrum UV light, while the competitor uses a different technology to produce broad spectrum UV light that covers the entire germicidal spectrum. The objection from the VA was clearly intended to protect the integrity of Dr. Jinadatha’s work, in light of Tru-D’s attempt to discredit Dr. Jinadatha to gain an advantage against Tru-D’s competitor.
UV light is becoming increasingly accepted as an effective tool in the battle against HAIs. The companies manufacturing and selling mercury UV devices need to be held accountable to provide hospitals with accurate information about these mercury UV devices to ensure employee and patient safety. Destroying the pathogens before they cause infections is what can and should be done TODAY. And it can be done safely without bringing more toxins into the hospital.
Mercury UV Vendor Shenanigans
-
A CDC-funded study proved the technology did not work against C.diff, MRSA or Acenitobacter infections.
-
Their bulbs contain mercury, which is toxic.
-
There are risks to patients and workers if the mercury bulbs break.
-
Mercury bulbs require special handling on disposal.
-
Mercury bulbs are very hot and require cool down time to avoid burns.
[PDF] references: EPA Cease and Desist Notice, DOI.org study, Germ-zapping robots studies, VA letter to Tru-D
Sources:
- The Lancet, Vol. 389, No. 10071, p805–814
- Quote from study author - Deverick Anderson during 2016 IDSA presentation: "Now given that we used bleach in all...we used bleach for terminal disinfection of all seed rooms with C.difficile. C. difficile outcome actually represents a comparison of bleach vs. bleach plus UV. And in our study we found no change in the rate of C. difficile after adding UV to bleach cleaning. Now turning to our secondary outcomes we evaluated the clinical incidence of MRSA in the four study arms. The clinical incidence/rate rate of MRSA was not significantly lower in any of the three enhanced strategies."
- Tru-D.com
Please contact us for more information.