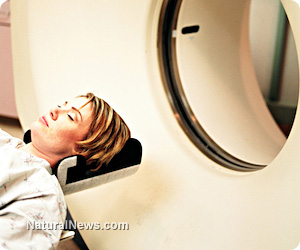
Brain scans show consciousness in vegetative patients
Thursday, May 01, 2014 by: David Gutierrez, staff writer
Tags: brain scan, vegetative patients, consciousness
- The best and worst forms of magnesium to take as a supplement
- Cinnamon and honey's healing properties
- Natural News Labs publishes heavy metals test results for seaweeds and sea vegetables: Kelp, Kombu, Wakame, Nori, Dulse and more
- The REAL FAKE NEWS exposed: '97% of scientists agree on climate change' is an engineered hoax... here's what the media never told you
- Pyroluria: The most common unknown disorder
- Deep Breathing can reduce stress, fatigue and high blood pressure
- Two men per day receiving prosthetic penis implants
- Apricot Seeds Kill Cancer Cells without Side Effects
- Gov't admits rotavirus vaccine causes intussusception, adds it to injury compensation program
- Five spices and herbs that really work for treating depression
- Sugar takes on high fructose corn syrup in high stakes legal battle to see which is most unhealthy
- Rickets on the Rise as Vitamin D Deficiency Surges Among Expectant Mothers
- Eight Remedies Treat Diabetes Naturally
- Choline Deficiency during Pregnancy may lead to Birth Defects
- Frankenscientists create GM 'supersniffer' mice with superpower senses
- The best homemade remedies to treat hay fever and seasonal allergies
- Magnesium and Atrial Fibrillation
- Health Ranger announces discovery, documentation of Metals Retention Factor for foods, superfoods, herbs and supplements
- The REAL FAKE NEWS exposed: '97% of scientists agree on climate change' is an engineered hoax... here's what the media never told you
- The remarkable health benefits of oil pulling
- The best and worst forms of magnesium to take as a supplement
- Water filters tested for heavy metals removal: Zero Water, Pur, Brita, Mavea, Culligan, Seychelle and Waterman
- Apricot Seeds Kill Cancer Cells without Side Effects
- Southern Poverty Law Center self-destructs into paranoid frenzy of leftist idiocy, naming nearly everyone a conspiracy theorist
- Indian black salve: The magical cancer cure
- Bill Gates says vaccines can help reduce world population
- Health Ranger announces discovery, documentation of Metals Retention Factor for foods, superfoods, herbs and supplements
- Baking Soda Prevents Kidney Disease, Renal Failure and Kidney Dialysis
- Inexpensive, easy detox - the one gallon challenge
- Beat cancer with 35% hydrogen peroxide
- The Bill of Rights is not negotiable - SHARE this urgent declaration
- Ten ways to use colloidal silver's amazing healing abilities
- Wisdom teeth surgery a deadly dental scam: Young mother falls into coma following visit to dentist
- Eliminate restless leg syndrome with home remedies and natural treatments
- Global warming data FAKED by government to fit climate change fictions
- U.S. supermarkets waste huge amounts of food
- The REAL FAKE NEWS exposed: '97% of scientists agree on climate change' is an engineered hoax... here's what the media never told you
- Bill Gates says vaccines can help reduce world population
- The best and worst forms of magnesium to take as a supplement
- Beat cancer with 35% hydrogen peroxide
- NASA admits to spraying Americans with poisonous chemtrails
- Water filters tested for heavy metals removal: Zero Water, Pur, Brita, Mavea, Culligan, Seychelle and Waterman
- The best, and worst, laundry detergents with 1,4-dioxane contamination
- Feeding the soil: An introduction to the no-till gardening method
- Peanut oil in vaccines behind widespread peanut allergy epidemic
- Study Reveals Serious HPV Vaccine Problems: Fainting, Blood Clots, Death Among Risks
- Eighteen Overlooked Symptoms of Adrenal Fatigue
- Apricot Seeds Kill Cancer Cells without Side Effects
- HPV vaccines are harming and killing victims worldwide in a silent epidemic of medical violence against children
- Six little-known natural remedies for tinnitus
- Forget Filling Cavities: Regrow Your Teeth Instead
- Five best homeopathic remedies for the treatment of heartburn, GERD and acid reflux
- The MMR vaccine, autism connection
- If carbon dioxide is so bad for the planet, why do greenhouse growers buy CO2 generators to double plant growth?
- Eleven days before Iran bombed Tel Aviv, my microscope revealed haunting images of EXACTLY what would happen
- Morphic resonance “remote viewing” reveals iconic Middle East images of stealth bombers, a falcon and a one-horned ram
- DECENTRALIZED SPIRITUALITY and the true teachings of Christ: Overcoming the censorship, threats and lies of organized religion to truly know God and the Universal Christ
- HEALTH SECRETS: How to Instantly Block MSG Toxicity Using Natural Substances (and the secret of Methylene Blue)
- Amazing microscopy photos reveal how freezing crystals attempt to mimic electronic structures they are touching
- The Coming Gold Revaluation: Strategic Financial Realignment in an Era of Dollar Collapse
- The AI Data Center Wars Have Begun… Farms, Water and Electricity is Stripped from Humans to Power the Machines
- Urgent Wake-Up Call: The Coming AI Robot Wars and the Great Human Unity
- The War on Light: How Governments and Big Pharma Keep You Sick By Blocking Healing Photons
- THE AI RACE IS ALREADY WON: How China’s power dominance (and America’s climate lunacy surrender) secured its victory in the race to AI superintelligence
- Why the U.S. Government May be Seeking to Slaughter 200 Million Americans to Free Up Excess Power for AI Data Centers and the Race to Superintelligence
- Trump's Trojan Horse: How Stablecoins Are Secretly Paving the Way for a CBDC Control Grid – an Interview with Catherine Austin Fitts
- EXCLUSIVE REPORT: The Trump-Putin Meeting in Alaska - A Historic Pivot that Redefined Global Power
- MSG EXPOSED: Hidden Neurotoxins Found in Groceries, Snacks and Popular Fast Food Menus
- BOMBSHELL: Internal Pfizer documents exposed and reveal at least 16 PERCENT of their mRNA vaccine "adverse events" are REPRODUCTIVE DISORDERS
- Shingles surge sparks new focus on holistic care: Tackling pain, immunity and risks
- Injecting chemicals is MORE DANGEROUS than eating them, so why is polysorbate 80 banned in ICE CREAM but allowed in VACCINES?
- BOMBSHELL: DNA testing kits are a SCAM to develop ethnic-specific bioweapons
"Our findings suggest that PET imaging can reveal cognitive processes that aren't visible through traditional bedside tests," lead researcher Steven Laureys said, "and could substantially complement standard behavioural assessments to identify unresponsive or 'vegetative' patients who have the potential for long-term recovery."
Current test unreliable
Doctors traditionally distinguish between comatose patients who are in a minimally conscious state (MCS) and those suffering from unresponsive wakefulness syndrome (a vegetative state). In an MCS, a patient still responds to some stimuli and shows some evidence of awareness; in a vegetative state, the patient is completely unresponsive and the chance of recovery has typically been considered very low.To distinguish between these two state, doctors rely on a standardized test called the coma recovery scale-revised (CSR-R). Unfortunately, CSR-R is only accurate about 60 percent of the time.
"In patients with substantial cerebral oedema [swelling of the brain], prediction of outcome on the basis of standard clinical examination and structural brain imaging is probably little better than flipping a coin," wrote Jamie Sleigh from the University of Auckland, New Zealand, and Catherine Warnaby from the University of Oxford in an accompanying commentary.
For the study, the researchers compared two separate, 3D diagnostic brain scan tools: a positron emission tomography (PET) scanner and a functional magnetic resonance imaging (fMRI) scanner. The PET scan functions by mapping the progress of a radioactive tracer (attached to glucose, the brain's energy source) through the blood as separate brain regions are activated by a stimulus. The fMRI scan functions by detecting the uptake of oxygen in various brain regions in response to a stimulus.
Over the course of four years, the researchers performed PET and fMRI tests on 81 patients who had been diagnosed via CSR-R as being in an MCS and 41 who had been diagnosed as being in a vegetative state. The tests were also performed, for comparison purposes, on 39 healthy people and four with "locked-in" syndrome (in which the brain is fully active but the person is unable to respond behaviorally).
"Far-reaching implications"
The researchers found that the PET scan was 93 percent successful at detecting MCS, while the fMRI was only 45 percent successful. In addition, the PET test was more effective than CSR-R in predicting eventual recovery.According to the CSR-R, 36 patients were completely unresponsive. However, the PET scan found brain activity consistent with MCS in 12 of these patients, nine of whom eventually recovered.
"PET imaging can reveal cognitive processes that aren't visible through traditional bedside tests," Laureys said.
The findings could significantly improve doctors' ability to determine the likelihood of patient recovery.
"This study is welcome because diagnosis and prognostic accuracy in patients with severe brain injury needs to be improved," Sleigh and Warnaby wrote. "For example, intensive care doctors caring for former racing driver Michael Schumacher after his recent serious brain injury refused to offer any firm prognosis to the world's media."
PET scanning could have implications for patients' families, as well.
"If the results of this study are confirmed in future research, this could have far-reaching clinical, ethical and legal implications," said Michael Bloomfield of the Medical Research Council, who was not involved in the study, " including whether to offer an apparently unconscious patient pain relief and, ultimately, whether treatments that may be keeping someone alive should be continued or not."
Sources for this article include:
http://www.newsdaily.com
http://www.sciencedaily.com
http://www.alphagalileo.org
http://science.naturalnews.com
Brain scan at FETCH.news
Get independent news alerts on natural cures, food lab tests, cannabis medicine, science, robotics, drones, privacy and more.
Take Action: Support Natural News by linking to this article from your website
Permalink to this article:
Embed article link: (copy HTML code below):
Reprinting this article:
Non-commercial use OK, cite NaturalNews.com with clickable link.
Follow Natural News on Facebook, Twitter, Google Plus, and Pinterest
Science News & Studies
Medicine News and Information
Food News & Studies
Health News & Studies
Herbs News & Information
Pollution News & Studies
Cancer News & Studies
Climate News & Studies
Survival News & Information
Gear News & Information
News covering technology, stocks, hackers, and more



"Big Tech and mainstream media are constantly trying to silence the independent voices that dare to bring you the truth about toxic food ingredients, dangerous medications and the failed, fraudulent science of the profit-driven medical establishment.
Email is one of the best ways to make sure you stay informed, without the censorship of the tech giants (Google, Apple, Facebook, Twitter, YouTube, etc.). Stay informed and you'll even likely learn information that may help save your own life."
–The Health Ranger, Mike Adams























